
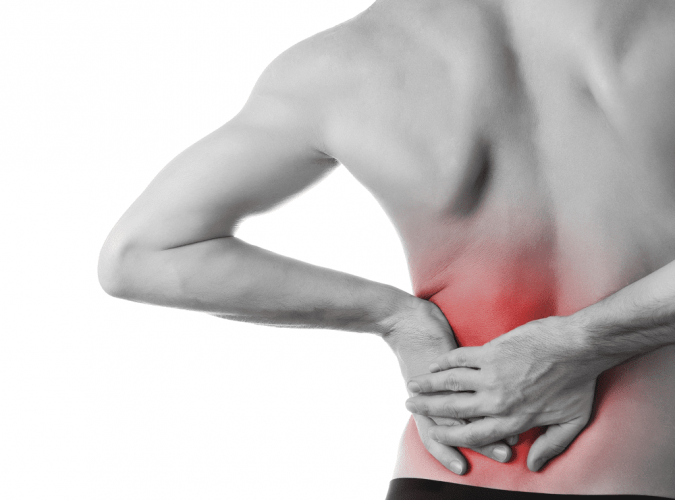
Specialists in the diagnosis, treatment and rehabilitation of the spine and pelvis.
Learn More
Delivering sport-specific injury assessment, treatment, rehabilitation and performance care.
Learn More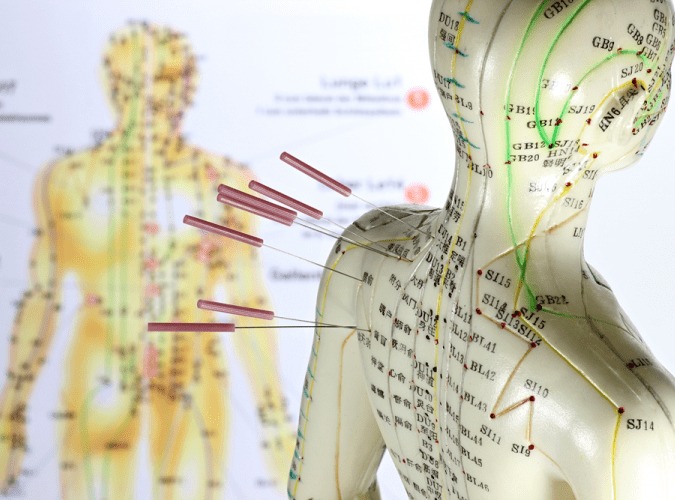
Acupuncture is an holistic approach to health and regards illness as a sign that the body is out of balance.
Learn More
Our sports massage practitioners techniques have been developed to ensure effective and efficient results.
Learn More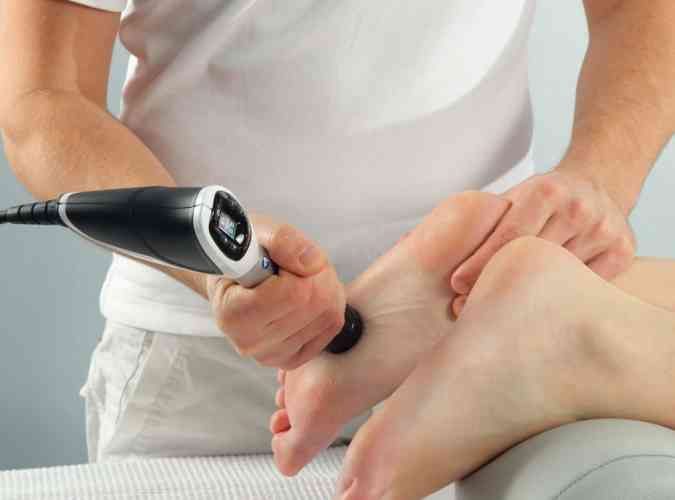
A revolutionary clinically proven and highly effective treatment for chronic soft tissue injuries.
Learn More


At our Liverpool Chiropractic Clinic we promise to provide undivided attention to your specific health and wellness needs. Every ache and pain in our bodies has an underlying cause. Though medication can offer temporary relief, it cannot correct functional problems of negatively affected spinal joints or unhealthy daily habits.
Liverpool Chiropractic Clinic specialise in the diagnosis, treatment and prevention of lower back pain, neck pain, headaches and sports injuries.
We utilise the most effective, cutting edge techniques to identify the true cause of your problem and develop personalised strategies to help you achieve optimum health and wellness.


“Excellent clinical care. I have never felt better. Having endured a stiff back with limited range of movement, I now find myself feeling so much more flexible leading to a better posture and a much improved range of movement in my back and hips. I have no hesitation in recommending Liverpool Chiropractic. I regret not going sooner.”
“Genuinely life-changing wizardry Years of back pain replaced with effective management and no fear of a relapse!”
“After suffering with back pain for around 2 months and seeing other back specialists with no joy I went to Liverpool Chiropractic after a recommendation from a colleague. They were so friendly and understanding and sorted me out very quickly, while explaining everything that was going on. Wouldn’t go anywhere else now!”

Doctor of Chiropractic

Doctor of Chiropractic

Doctor of Chiropractic

Doctor of Chiropractic

Sports Injury Therapist

Sports Injury Therapist

Sports Injury Therapist / Operations Manager

Sports Injury Therapist

Sports Injury Therapist / Business Support

Practice Manager

Doctor of Chiropractic

Doctor of Chiropractic

Doctor of Chiropractic

Doctor of Chiropractic

Sports Massage Therapist

Lorem ipsum, dolor, sit amet consectetur adipisicing elit. Accusamus incidunt aperiam atque. Soluta quia voluptate, accusantium quos maxime odio similique architecto voluptas voluptatem odit libero, blanditiis, nesciunt exercitationem ipsa commodi!
So you can run after the kids all day, pick your grandchildren up, enjoy a round of golf, run and walk with ease, get back to the gym and breaking some PR’s in your races.
So you’re not relying on painkillers to get through the day, knowing that its just masking the problem, but you have no choice, even though it’s no good for long term health.
We’ll help you get to the root cause of your problem before its too late and are facing surgery, because you can’t take it any more.
We’ll help give you clarity and peace of mind that your problem is being taken care of and you’ll have the guidance, strategies and exercises to speed up your recovery and keep long term results.
So you can enjoy quality time with friends and family that the aches and Pains steal from you, and finally get a good nights sleep without tossing and turning trying to find that one position that feels comfortable.
Basically, we love to help people just like you, move better, feel better and live better – free of painkillers and the curse of chronic pain…
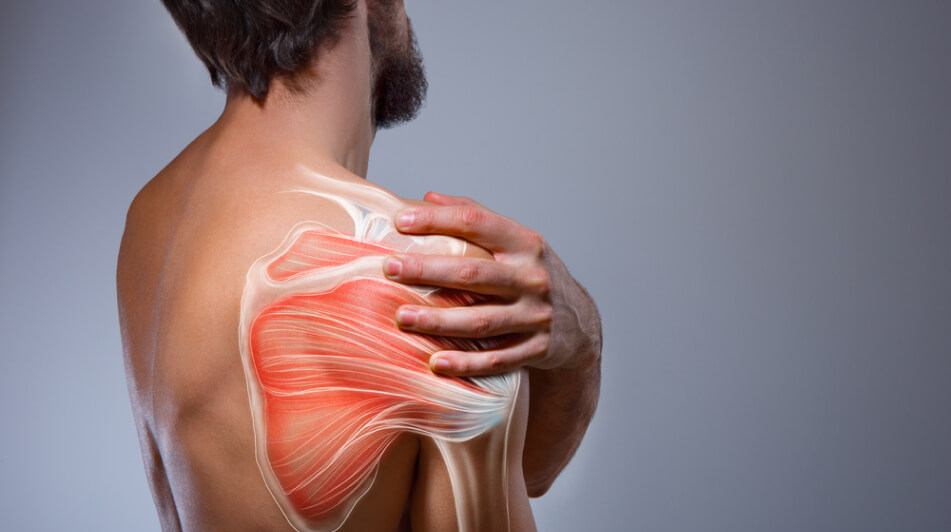
We Pride ourselves on providing exceptional care for people just like you who want to be more active and mobile, free from painkillers, without fear of pain holding you back.
If any of this sounds like you - we would love to help you at one of our clinics.
We've helped so many people just like you, who have all gone through the same thing.
Click the link below to speak to one of our team.
There is no obligation to book any appointments with us after the call is over. Our goal is to help you make the right decision about what to do next for the best .
We Pride ourselves on providing exceptional care for people just like you who want to be more active and mobile, free from painkillers, without fear of pain holding you back.
If any of this sounds like you - we would love to help you at one of our clinics.
We've helped so many people just like you, who have all gone through the same thing.
Click the link below to speak to one of our team.
There is no obligation to book any appointments with us after the call is over. Our goal is to help you make the right decision about what to do next for the best .
See how the chiropractic Team at Liverpool Chiropractic Clinic can help you move better, feel better and live better – by clicking the button below and calling our team.


"*" indicates required fields

"*" indicates required fields

"*" indicates required fields